CHRONIC OBSTRUCTIVE AIRWAYS DISEASES
Chronic Obstructive Airways Diseases (COPD) is a lung disease that includes —
1. Respiratory failure
2. Bronchitis
3. Emphysema
Respiratory Failure
Respiratory failure is inadequate gas exchange by the respiratory system, with the result that levels of arterial oxygen, carbon dioxide or both cannot be maintained within their normal ranges. A drop in blood oxygenationis known as hypoxemia; a rise in arterial carbon dioxide levels is called hypercapnia. The normal reference values are: oxygen PaO2 more than 80 mmHg (11 kPa), and carbon dioxide PaCO2 lesser than 45 mmHg (6.0 kPa). It is classified into type I or type II which relates to the absence or presence of hypercapnia respectively.
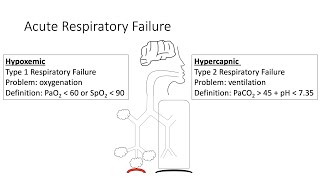
Hypoxemic respiratory failure (type I):
It is characterized by an arterial oxygen tension (Pa O2) lower than 60 mm Hg with a normal or low arterial carbon dioxide tension (Pa CO2). This is the most common form of respiratory failure, and it can be associated with virtually all acute diseases of the lung, which generally involve fluid filling or collapse of alveolar units. Some examples of type I respiratory failure is cardiogenic or non-cardiogenic pulmonary edema, pneumonia and pulmonary hemorrhage.
Hypercapnic respiratory failure (type II): It is characterized by a PaCO2 higher than 50 mm Hg. Hypoxemia is common in patients with hypercapnic respiratory failure who are breathing room air. The pH depends on the level of bicarbonate, which, in turn, is dependent on the duration of hypercapnia. Common etiologies include drug overdose, neuromuscular disease, chest wall abnormalities, and severe airway disorders (e.g, asthma and chronic obstructive pulmonary disease).
Causes
Common causes of type I (hypoxemic) respiratory failure include the following:
• Pneumothorax
• Pulmonary embolism
• Pulmonary arterial hypertension
• Pneumoconiosis
• Granulomatous lung diseases
• Cyanotic congenital heart disease
• Bronchiectasis
• Acute respiratory distress syndrome (ARDS)
• Fat embolism syndrome
• Kyphoscoliosis
• Obesity
Symptoms
A majority of patients with respiratory failure are short of breath. Both low oxygen and high carbon dioxide can impair mental functions. Patient may become confused and disoriented and find it impossible to carry out their normal activities and work.
- Marked CO2 excess can cause headaches
and, in time, a semiconscious state, restlessness, anxiety, confusion, seizures, or even coma. - Polycythaemia is a complication of long- standing hypoxaemia.
• Corpulmonale (failure of the right side of the heart): Pulmonary hypertension is frequently present and may induce right ventricular failure, leading to hepatomegaly and peripheral oedema.
• Physical examination may show a patient who is breathing rapidly, is restless and has a rapid pulse.
• Lung disease may cause abnormal sounds; wheezing in asthma, “crackles” in obstructive lung disease.
Complications
• Pulmonary fibrosis.
• Collapsed lung (pneumothorax).
• Blood clots.
• Infections.
• Abnormal lung function.
• Memory, cognitive and emotional problems.
Treatment
The goals of treatment for respiratory failure are to increase oxygenation and
improve ventilation. Treatment depends on the severity of the respiratory failure and the cause. Acute respiratory failure treatment will address the underlying cause and include ventilation and oxygenation as needed. Exacerbation of chronic respiratory failure by infection may require hospitalization, and treatment may include oxygenation and ventilator Bronchodilators may improve patency.
support airway.Multiple options are available for the treatment of respiratory failure. Examples include:
• Antibiotics to prevent and treat respiratory infections.
• Bi-level positive airway pressure (BiPAP).
• Bronchodilators, like anticholinergics, such as tiotropium or β-agonists, such
as Albuterol.
• Continuous positive airway pressure (CPAP).
• Inhaled steroid medications to decrease inflammation
• Mechanical ventilation, if oxygen therapy is not sufficient to increase blood oxygen levels.
• Oxygen therapy to increase blood oxygen levels.
• Tracheostomy, a hole made in the front of the neck to help breathing.
• A patient whose breathing remains very poor will require a ventilator to aid
breathing.
• Suctioning the lungs through a small plastic tube passed through the nose, in order to remove secretions from the airways that the patient cannot cough up.
.png)
















.jpg)
.png)






